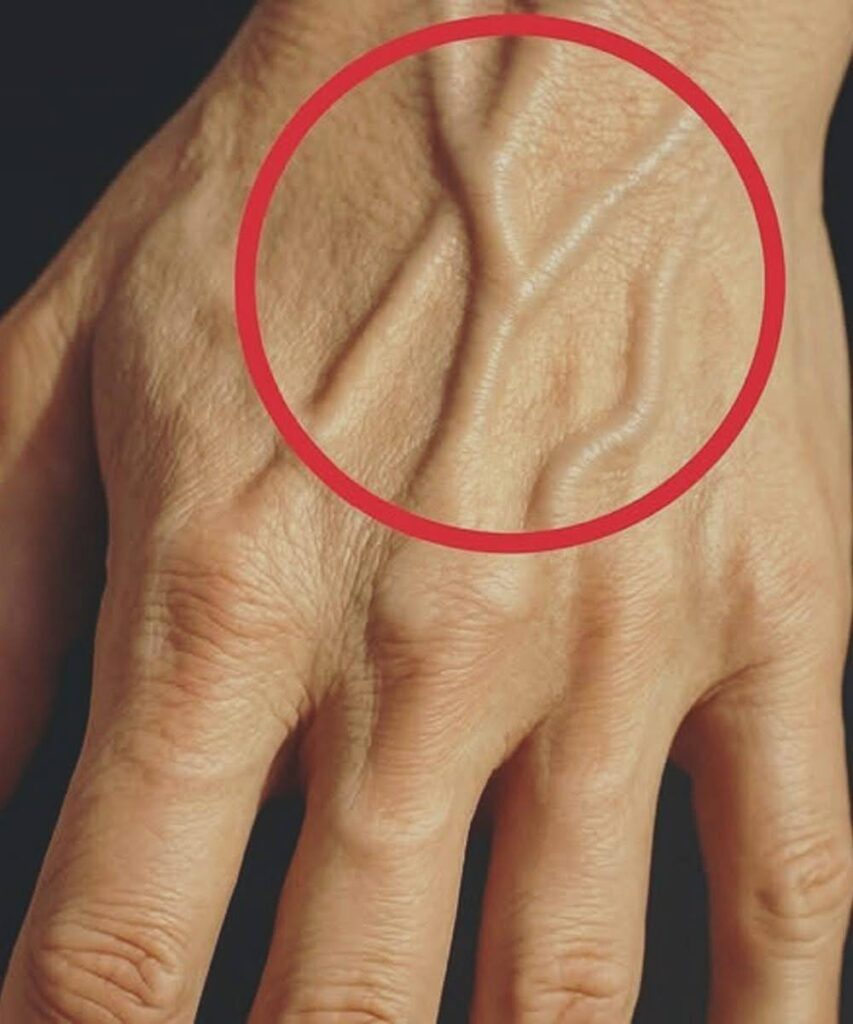
Have you ever noticed bright blue veins popping out on the back of your hands and wondered whether that’s simply cosmetic or a sign of something more serious happening beneath the surface?
Visible veins are a common physical trait many people notice, especially when hands are exposed, skin is thin, or the lighting makes the vein color stand out more than usual.
These veins are part of the superficial venous network, which lies just below the skin and is responsible for returning deoxygenated blood back toward the heart after it delivers oxygen to tissues.
The color you see — often blue, greenish, or teal — isn’t the actual blood color but rather how light penetrates the skin and reflects back from the vein surface and surrounding tissue.
People with lighter skin tones and less subcutaneous fat frequently see their veins more clearly, because there’s less tissue between the skin surface and the veins themselves.

Aging also contributes to more prominent veins, as skin becomes thinner and loses elasticity over time, allowing the underlying veins to show through more easily than in younger skin.
When you bend your wrist, clench your fist, or raise your arms overhead, the veins can become even more visible due to increased blood flow and muscle contraction pushing veins toward the surface.
Some individuals are naturally predisposed to visible veins due to genetics;
family traits influence vein size, depth, and how closely they lie under the skin’s surface.
Athletes and physically active people — especially weightlifters — often develop bulging veins through consistent muscular development that compresses veins and increases blood flow during exercise.
During physical activity, veins expand to accommodate greater blood volume, which can make them appear larger and more prominent on the hands, arms, and other limbs.95
Pregnancy also leads to increased vein visibility because the circulatory system expands to support the growing fetus, raising blood volume and pressure in certain vessels.
Women who are pregnant often develop visible veins on hands, arms, or legs, and these changes usually improve after childbirth as cardiovascular conditions normalize.
Environmental factors like heat can dilate blood vessels, making veins more visible as the body adapts to maintain proper internal temperature and blood flow.
Dehydration can also make veins appear more pronounced because reduced fluid levels shrink the volume beneath the skin, increasing vein contrast against the surface.
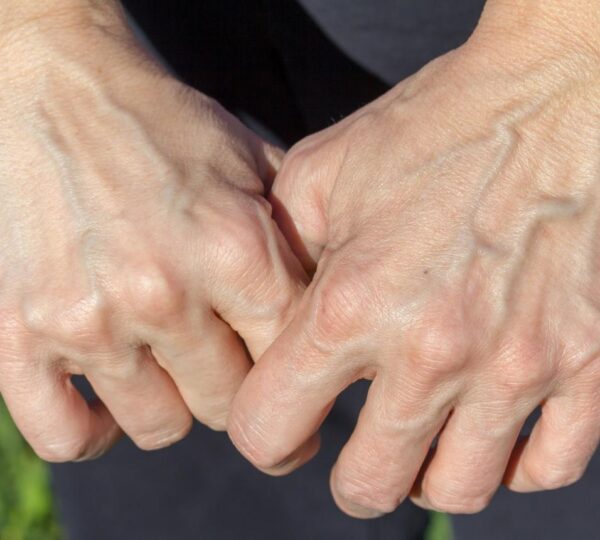
While most visible blue veins are benign and reflect normal anatomy, there are times when changes in vein appearance should prompt medical evaluation.
One common vein condition is varicose veins, which occur when vein walls weaken and valves fail, causing blood to pool and the veins to become enlarged, twisted, and rope‑like.
Varicose veins are most often seen in the legs and feet but can occasionally occur on hands if local vein structure and circulation are affected by age or repetitive use.
Symptoms of varicose veins can include aching, heaviness, burning, throbbing, or swelling, especially after long periods of standing or sitting.
Varicose veins are more common in adults over age 50, people with a family history, individuals who are overweight, and women who have experienced multiple pregnancies.
Risk factors also include prolonged standing or sitting, hormonal changes, and occupations that require long hours on the feet without movement or breaks.
Unlike superficial cosmetic veins, deep vein issues can be serious and require medical attention, particularly if there is sudden swelling, pain, warmth, or redness along the vein path.

One condition of concern is deep vein thrombosis (DVT), in which a blood clot forms in a deep vein, typically in the legs, but sometimes in the arms, and can be dangerous if dislodged.
Symptoms of DVT may include persistent swelling, localized pain, warmth, discoloration, and veins that feel tender beneath the skin, especially after inactivity or long travel.
A potentially life‑threatening complication of DVT is pulmonary embolism, which happens when a clot travels to the lungs and blocks blood flow, requiring emergency medical care.
Other warning signs that warrant prompt evaluation include sudden onset of enlarged veins, noticeable skin changes, or symptoms that worsen over days rather than hours.
Some vascular conditions, such as superficial thrombophlebitis, involve clots in veins closer to the skin and may cause redness, warmth, pain, and visible swelling along the affected vein.
Although superficial thrombophlebitis is usually less dangerous than DVT, it still merits medical assessment and appropriate treatment to prevent progression or complications.
Visible veins may sometimes be linked to venous insufficiency, where weakened vein valves allow blood to flow backward, leading to pooling and increased vein visibility at rest.
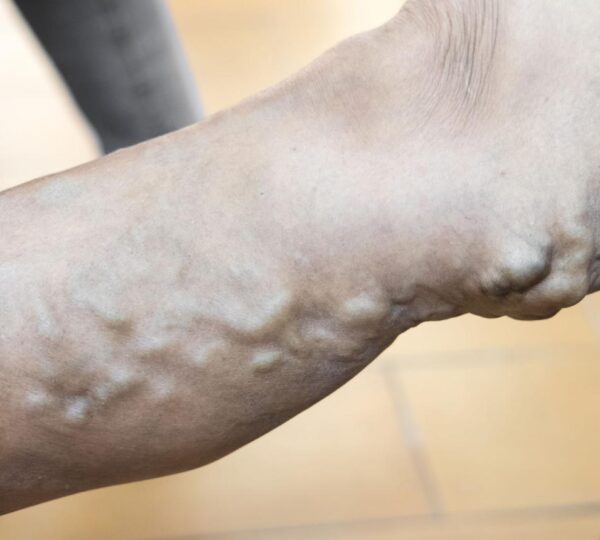
Symptoms of venous insufficiency include aching, heaviness, swelling, skin changes, and in more advanced cases, ulcers around the ankles or lower legs.
Healthcare providers can evaluate vein health using ultrasound imaging, which allows visualization of blood flow, vein structure, and valve function without invasive procedures.
Understanding when veins are simply visible versus when they reflect underlying problems comes down to evaluating symptoms, risk factors, and recent changes over time.
For many people, visible veins are a normal variation in anatomy and physiology, especially if there are no associated symptoms like pain or swelling.
In fact, vascular specialists note that prominent veins alone — without symptoms — rarely indicate a serious health problem and often do not require treatment.
However, if you notice persistent discomfort, unusual swelling, warmth, or rapid changes in vein appearance, it is wise to consult a healthcare provider for personalized evaluation.
Healthy lifestyle measures support overall vein and circulatory health and can also reduce discomfort for people prone to visible veins or mild varicose changes.
Regular physical activity — such as walking, swimming, or cycling — encourages healthy circulation and reduces pressure buildup in veins that can contribute to prominence or discomfort.

Maintaining a healthy weight lowers mechanical stress on the vascular system, which may lessen symptoms and improve overall vein function over time.
Avoiding long periods of sitting or standing without movement is important; taking short walking breaks or gently stretching improves blood flow in the limbs.
Smoking cessation is critical because tobacco use damages blood vessels, promotes inflammation, and increases the risk of vascular issues, including varicose veins and clot formation.
Wearing loose‑fitting clothing, especially around the waist, legs, and arms, helps minimize external pressure on veins and supports comfortable circulation throughout the day.
Some people find that elevating limbs periodically, such as propping hands or feet up while resting, helps reduce swelling and encourages venous blood flow back toward the heart.
For those with symptomatic varicose veins, treatments range from supportive measures like compression stockings to supervised outpatient procedures that improve venous function.
Compression stockings apply gentle pressure on the legs or arms to enhance venous return and reduce pooling, and they are often recommended as a first‑line therapy.
Medical procedures for varicose veins include sclerotherapy, in which a solution is injected into the vein to collapse it, redirecting blood flow to healthier vessels.
Other treatments may include endovenous laser therapy (EVLT) or radiofrequency ablation, which use heat to seal problematic veins and encourage blood flow through healthier routes.
In more severe cases, surgical options such as vein ligation and stripping may be considered, though these are typically reserved for extensive or refractory disease.
Recovery from such procedures varies by individual but often involves minimal downtime with guidance from a vascular specialist about gradual return to activity.
Even though some vein treatments improve appearance, their primary goal is to reduce symptoms, prevent progression, and support healthy circulation long term.
Nutritional factors also influence vein and cardiovascular health; diets rich in fruits, vegetables, lean proteins, and healthy fats provide antioxidants and nutrients that support blood vessels.
Staying well hydrated supports normal blood volume and flow, which can help veins function efficiently and reduce excessive prominence caused by dehydration.
Some supplements — like flavonoids found in citrus fruits — are studied for potential vein health benefits, but always consult a healthcare provider before starting any new regimen.
Age, genetics, lifestyle, and occupation all play roles in how visible veins appear and whether they cause discomfort or remain purely cosmetic.
Vascular health specialists emphasize that most cases of blue, visible veins are normal anatomical variations that do not require intervention unless accompanied by symptoms.
The Cleveland Clinic and other trusted medical sources note that visible veins are a common experience, especially in adults who are thin, active, or have naturally lighter skin tones.
Approximately one in three adults develops some form of varicose veins during their lifetime, underscoring how common venous visibility and changes can be.
Even in people with varicose veins, many experience only mild symptoms that do not interfere with daily activities and can be managed conservatively.
But ignoring warning signs such as pain, swelling, sudden changes, or signs of infection or inflammation is unwise; these symptoms can point to underlying vascular conditions.
Regular check‑ups with a primary care provider or vascular specialist help monitor vein health and circulation, especially in people with risk factors like family history or sedentary work patterns.
Many people find that discussing symptoms early leads to more tailored, effective care and reassurance when veins are simply prominent rather than problematic.
Visible veins may be telling you something about your circulatory system, but not every visible vein signals danger — context and symptoms matter.
If in doubt, seeking a medical opinion provides clarity, peace of mind, and a roadmap for maintaining vascular health over the long term.
Your veins support an essential function: returning blood to the heart efficiently and quietly, even when they show up more clearly than you expected.
Understanding the many reasons veins become visible — anatomy, activity level, aging, or underlying venous conditions — empowers you to make informed health decisions.
Whether veins are simply part of your natural physique or your body is signaling a vascular issue, awareness and informed care are your best allies.
Ultimately, prominent blue veins can be normal, natural, and harmless — but if they throb, burn, or change quickly, that’s a cue to talk with a doctor.
Health professionals are there to help interpret your body’s signals, support healthy circulation, and ensure your vein health stays on track.
Your vascular system is complex and resilient, but it deserves attention when something feels amiss or unlike your usual baseline.
Visible veins can be fascinating, functional, and sometimes concerning — understanding both normal variations and warning signs empowers better lifelong health.
If you notice new symptoms or pain, don’t hesitate to get checked — your veins might be revealing something important about your heart and circulation.
Healthy habits, regular movement, and thoughtful medical evaluation when needed help keep veins functioning as they should throughout life’s many chapters.
